

She Was Denied Wegovy 3 Times. Then She Found This $67/Month Alternative. And Lost 31 Lbs in 5 Months.
After 11 years of failed diets and a fourth insurance denial, Linda stumbled onto the same biological pathway that makes semaglutide effective. and it changed everything.

It was the fourth time Linda had been denied.
She sat in the CVS parking lot with her phone in her lap, the hold music still ringing in her head. The insurance rep had been polite — they always were. “We’re sorry, but your current BMI score doesn’t meet the criteria for coverage of this medication.”
She typed the same search she’d typed a dozen times before: Wegovy alternative that actually works.
She’d tried everything. Not casually tried — seriously, obsessively tried. Keto for 7 months. Noom for a year and $200. Two separate Weight Watchers cycles. She wasn’t someone who gave up. She was someone who was running out of options.
What she found that night, in a research article buried under 14 pages of Google results, wasn’t a weight loss supplement. It was an explanation — finally — for why her hunger was different from everyone else’s.
Why Willpower Has Nothing to Do With It
You’re not lazy. You’re not lacking willpower. And you’re definitely not “broken.” If it feels like you’re constantly fighting your own hunger, thinking about food all day, never quite feeling satisfied, watching other people eat “normally” while you’re battling cravings every few hours that frustration is real. Most people have been taught that weight gain is simply about discipline, but the truth is your biology plays a massive role in how hungry, full, and in-control you feel every single day.
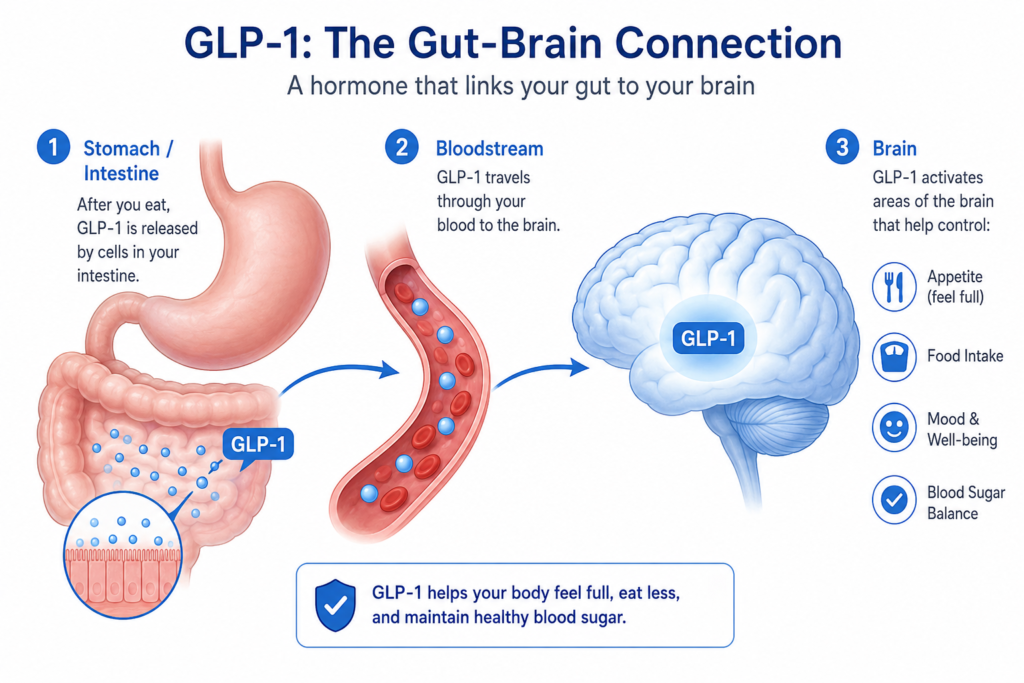
One of the biggest drivers behind that struggle is a hormone called GLP-1. This naturally occurring hormone is produced in your gut and helps regulate appetite, blood sugar, digestion, and fullness signals between your stomach and brain. When GLP-1 is working properly, your body can recognize when you’ve had enough food. Hunger becomes quieter. Cravings become manageable. You stop obsessing over your next meal because your brain finally receives the message that you’re nourished and satisfied.
“When GLP-1 levels are chronically low, your brain literally cannot receive the ‘I’m full’ signal — no matter how much you eat.”
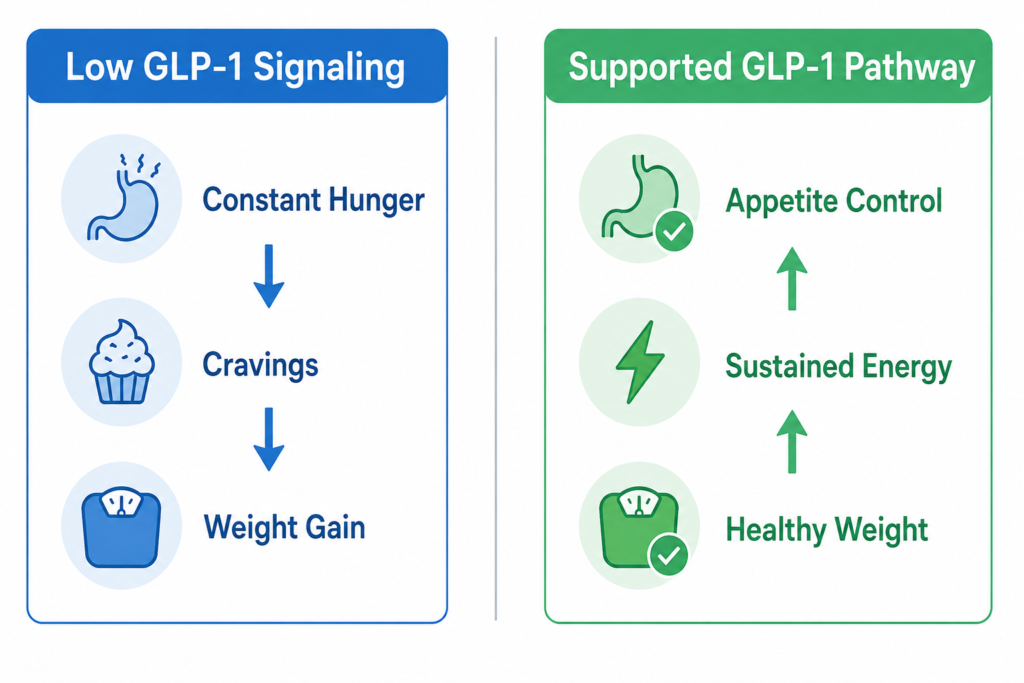
When GLP-1 levels stay low for long periods of time, your entire hunger system can feel out of sync. Food leaves the stomach too quickly, blood sugar spikes and crashes harder, and the brain keeps sending “eat more” signals even after a full meal. That’s why so many people describe feeling hungry again an hour after eating, constantly snacking without satisfaction, or losing weight temporarily only to gain it all back. It’s not simply a motivation problem, it’s a hormonal signaling problem that can make your body work against you around the clock.
Why Everything You've Tried Has Failed (And Why That's Not Your Fault)
Calorie Restriction
At first, cutting calories can seem effective because eating less often creates an initial drop in weight. But calorie restriction alone doesn’t repair the underlying GLP-1 signaling problem, so your brain may still feel deprived and intensely hungry. Over time, that constant biological drive to eat can become exhausting, making the approach feel impossible to sustain long-term.
Keto / Low Carb
Low-carb diets can temporarily reduce cravings and stabilize blood sugar, which is why many people feel better in the beginning. But for many people, the deeper GLP-1 deficiency is still there beneath the surface, meaning fullness cues never fully normalize. Eventually, hunger, food fixation, or rebound overeating can return once the diet becomes harder to maintain in real life.
Appetite Suppressants
Appetite suppressants may seem helpful because they temporarily blunt hunger signals and reduce how much you want to eat. The problem is that many of them don’t truly restore the body’s natural GLP-1 communication system — they simply override it for a short period of time. Once the effect wears off, the original hunger signaling often comes rushing back, leaving people feeling frustrated and defeated.
Diet Programs
Structured diet programs can feel motivating because they provide rules, accountability, and a clear plan to follow. But even the “perfect” plan can become overwhelming when low GLP-1 levels are still telling your brain you’re hungry all the time. That’s why so many people blame themselves for “falling off track,” when in reality their biology was making the process far harder than it should have been.
Then the 2023 Yale Research Revealed Something Most Doctors Never Discuss With Their Patients
The hormone at the center of this entire conversation is called GLP-1, short for glucagon-like peptide-1. It’s a naturally occurring hormone released in your gut after you eat, and its job is to coordinate communication between your digestive system, pancreas, and brain. GLP-1 helps regulate appetite, slows how quickly food leaves the stomach, supports healthy insulin release, and most importantly, tells your brain when you’ve had enough food. When this signaling pathway functions properly, hunger feels calmer, portions feel naturally satisfying, and the constant mental “food noise” begins to quiet down. (Reddit)
Here’s the critical part most people never hear: when GLP-1 signaling is impaired or chronically low, your body can start working against you. The stomach empties faster, blood sugar becomes more unstable, cravings intensify, and the brain struggles to register fullness correctly. That’s why so many people feel hungry shortly after eating or describe an almost nonstop preoccupation with food despite trying hard to “eat better.” This is not simply about discipline — it’s about biological messaging between the gut and the brain. Peer-reviewed research has repeatedly shown that GLP-1 plays a central role in satiety, glucose regulation, and metabolic control. (PubMed)
Researchers have also identified certain natural compounds that may help support or stimulate GLP-1 activity. One of the most studied is berberine, a plant-derived compound traditionally used in metabolic health research. Multiple studies found that berberine can stimulate GLP-1 secretion in intestinal cells through gut receptor pathways and may also support GLP-1 production at the cellular level. Other compounds being explored for GLP-1 support include curcumin, probiotics, omega-3 fatty acids, and certain bitter plant polyphenols that interact with gut signaling pathways. (PubMed)
What makes this approach different is that instead of relying purely on restriction, stimulant-based appetite suppression, or endless dieting rules, the goal is to support the body’s own satiety signaling mechanisms directly. Rather than fighting hunger every hour of the day, the focus becomes helping your biology communicate properly again — so fullness feels more natural instead of forced. That distinction matters because sustainable weight management becomes dramatically easier when your brain and body are finally receiving the same signals.
It’s also important to stay realistic and evidence-based. Natural compounds like berberine are not identical to prescription GLP-1 medications and should not be presented as direct pharmaceutical equivalents. However, emerging research suggests they may help support some of the same metabolic pathways involved in appetite regulation and blood sugar balance. In other words, this product isn’t designed to “override” your body through sheer suppression — it’s designed to work with the body’s existing hormonal signaling systems in a more supportive, physiology-based way. (Fella Health)
After Reviewing the Research, One Formula Met Every Clinical Criteria
After learning how important GLP-1 signaling is for appetite, cravings, and fullness, many people start looking for ways to support those pathways naturally — which is exactly why products like [PRODUCT NAME] have been getting so much attention lately. Instead of focusing on harsh restriction or stimulant-heavy appetite suppression, the formula is designed to work with the body’s existing metabolic and satiety systems. For people who feel like they’ve spent years fighting constant hunger and food noise, that difference can feel surprisingly meaningful.
The formula combines three key ingredients often associated with metabolic and appetite-support pathways: berberine, which has been studied for its potential role in supporting GLP-1 activity and healthy blood sugar balance; chromium, which may help support insulin sensitivity and reduce energy crashes that trigger cravings; and cinnamon extract, traditionally used to support glucose metabolism and steadier appetite signaling. Together, these compounds are intended to help support a calmer hunger response, fewer intense cravings, and a more stable feeling of fullness throughout the day — so eating less doesn’t feel like a constant battle of willpower.
While some people are surprised by how affordable this type of metabolic support can be compared to expensive programs or prescriptions, availability has been changing quickly as awareness grows. If you want to see the latest details, ingredient breakdowns, and real customer experiences for yourself, you can check the official page below.
Check current availability and read 2,847 verified buyer reviews →

"I spent 3 years telling myself I just needed more willpower. What I actually needed was someone to explain that my GLP-1 hormone was low. In 8 weeks, the constant hunger I've had since my 40s just... quieted down. I've lost 18 lbs and I'm not even thinking about food constantly anymore."

"My doctor suggested Wegovy but my insurance refused to cover it. A friend sent me this article. I started the formula 11 weeks ago. Down 23 lbs. I told my doctor and she asked me what I was taking."

"I was skeptical of anything that mentioned GLP-1 because I assumed it was just marketing. But this article explains the actual science — and the product does exactly what the science says it should. 4 months in, 27 lbs down."

See the Full Formula, Clinical Ingredients, and 2,847+ Verified Buyer Reviews

